Mesh Complications Patient Story 43
Vaginal Pain, Painful Sex & Right Lower Abdominal Pain following Sacral Colpopexy with Mesh
Mesh Complications: Vaginal Pain, painful sex, right lower abdominal pain, and a 'rubbing sensation' in the vagina
Treatment: Laparoscopic removal of Sacral Colpopexy Mesh
In 2008, this 55-year-old woman had an open (i.e. large incision) sacral colpopexy performed in her home state of Virginia. After the surgery, she suffered from a great deal of pain and discomfort. She followed up with her surgeon as prescribed, who reportedly stated, “There is nothing wrong with you nor can I do much to help you.” In October of 2011, she consulted her surgeon again. The surgeon recommended physical therapy, pelvic massage, and a hormone specialist.
It was during this time that the patient reported seeing multiple advertisements related to class action lawsuits regarding mesh. Frustrated that her symptoms were not improving, she sought out the care and expertise of Drs. Miklos & Moore in Atlanta, GA for potential surgery. After consultation and consent, the patient was taken to the operating room on January 31, 2012. The patient underwent the following procedures:
- - Adhesiolysis - aka the cutting down of internal scar tissue
- - Laparoscopic removal of the sacral colpopexy mesh
- - Laparoscopic repair of her prolapsed bladder (i.e. cystocele) – paravaginal repair
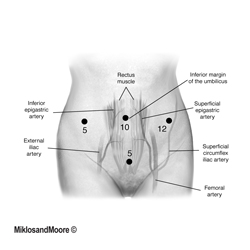
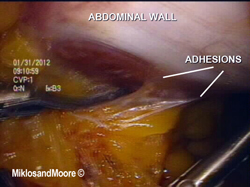
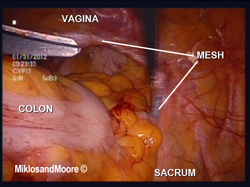
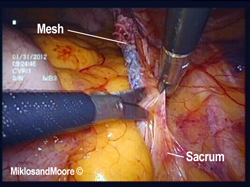
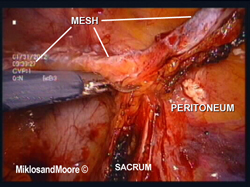
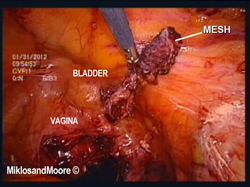
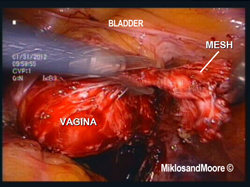
The surgery was performed laparoscopically (i.e. mini incisions) (Figure 1). Once inside the abdominal cavity the adhesions were removed (Figure 2, Photo 2 of the operative report). The mesh was identified between the vagina and the sacrum (aka tailbone). The peritoneum over the mesh was incised . The mesh was slowly dissected away from the sacrum and adherent tissue until the mesh was removed from the hollow of the sacrum . The final dissection was the removal of the mesh from the vagina . Figure 8 shows the mesh removed from the patient’s body.
The patient did well post operatively. However, she did develop an ileus (bowel obstruction) seven days after the surgery and was admitted to a Virginia hospital. The patient was discharged after three days stay and is currently doing well.